Angela Hospice Celebrates National Social Work Month
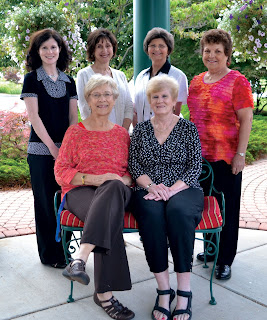
In honor of National Social Work Month we took a few minutes to talk with Angela Hospice’s Director of Social Work and Bereavement, Rebecca DeRaud, to learn why this team works so well together, what it’s been like to watch them grow, and more. Check it out! Rebecca (top left) with the Angela Hospice bereavement team. How long have you worked here? Sixteen years this June. How many social workers were here when you started? There were three. There’s one remaining from then, besides me, and now there are 20 of us all together. What’s it been like to see that growth over the years? It’s been a phenomenal experience. In many ways I feel like we’re all growing up together. We’ve all watched each other and we’ve all helped each other become better clinicians, further each other’s professional development, and definitely personal development too. What makes an Angela Hospice social worker unique? What I think makes them unique is that they have excellent clin...